Sponsor a Star: Headsets take patients away from their pain
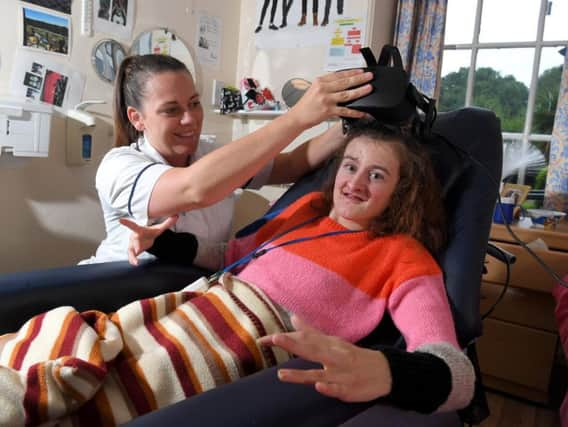

Heather Barker smiles and slowly relaxes into her chair as she is transported into another world.
She can almost feel the jeep move underneath her as it drives down the track on safari.
Advertisement
Hide AdAdvertisement
Hide AdIt pulls up to a herd of giraffes stretching their long necks to chomp at the highest leaves on the tree.


As Heather, wearing a virtual reality (VR) headset, is taken off on an Africa trek, Sue Ryder Neurological Care Centre physio at Cuerden Hall Sinead Gallery picks up one of Heather’s arms and starts to ease it into a stretch.
Her body, which is often tense, is more pliable now that she is elsewhere, distracted and calm, enjoying her virtual safari.
It’s an experience she may not otherwise have in reality as Heather has juvenile Huntington’s disease.
Advertisement
Hide AdAdvertisement
Hide AdShe is one of the residents at Cuerden Hall who would benefit from Sponsor a Star donations for a bespoke virtual reality headset, one of the items on the Christmas wish list we want to raise money for at the new specialist care centre coming to Fulwood.


The team at Sue Ryder are piloting a project to see if VR can help people living with neurological conditions. They say the effect on Heather was remarkable.
“It’s just to see if the virtual reality helps reduce pain or anxiety and improves people’s mood or behavioural problems,” says Sinead.
“Heather was one of the first we tried it on. She was really keen to start but I didn’t expect her reaction.
Advertisement
Hide AdAdvertisement
Hide Ad“She’s got quite a lot of uncontrolled movements but when we put it on her she literally just relaxed down.


“We could not believe it because we’d not had that from Heather before.
“When we were asking her about what she enjoyed she just said it’s relaxing.
“We had another resident who said ‘it just gave me the chance to escape from reality’.” Sinead says that if she was able to use the VR headset on some of her patients while she helped them stretch out their arms and legs “we could get even better results”.
Advertisement
Hide AdAdvertisement
Hide AdShe adds: “We might carry out passive stretches for them so what that means is that we are doing the stretching for them to stop the joints becoming contracted.

“For people with long term conditions who might not be able to get up and walk again or make a drink, it makes it more comfortable for them.
“If they weren’t getting those passive stretches the muscles would seize up, they would get tighter and even personal care like getting them up and dressed would become a real issue.
“It’s maintaining their range of movement to make personal care easier. But also they get pain if they’re not moving so it helps reduce that. Some of these conditions don’t improve, they get worse. It’s just trying to make it easier for them.”
Advertisement
Hide AdAdvertisement
Hide AdAsked if the VR headset made her feel as though she was in Africa on safari or if the underwater scene made her feel as though she were scuba diving Heather gave the thumbs up, indicting “yes”.
Care and admin worker Amy Philipson said: “When Heather had the VR headset on she was completely still and relaxed. It was great.
“The physio came and got me and said look at how well Heather’s doing.


“The physio’s idea was that because some people don’t get out to do these things it’s kind of like they are missing the chance so you can give them that experience and it’s realistic to them as well.”
Advertisement
Hide AdAdvertisement
Hide AdGeorge, Heather’s grandfather, was really keen to hear about how she had taken to the VR experience.
“That’s fantastic,” he said, when he heard of how her involuntary movements calmed when she wore the headset.
He added: “She’s starting to seize up a bit at the moment.
“It would help her wellbeing and would put her into a new world for a little while.”
Lead nurse Fiona Hinde is equally excited about the potential of VR to help patients.
Advertisement
Hide AdAdvertisement
Hide Ad“Residents with Huntington’s can be quite agitated and they don’t communicate but you just put the VR headset on and you can just see them settle so they’re obviously getting something out of it.
“Their body language says its relaxing and calming them. It’s just a bit of escapism.”
Centre director Terry Mears says the possibilities for using VR are incredible. “What’s really interesting is the way the brain can recreate the neuro pathways that had previously been damaged,” he says.
“It takes us to a place that we have never been before around people’s potential - post-acute episode.
Advertisement
Hide AdAdvertisement
Hide Ad“The research is still ongoing but we see the technology as key going forward.
“In post acute phase for example if the focus is on enabling people to walk again or gaining maximum control of their limbs there are certain programmes that, through the VR, will stimulate the new pathways within the brain where the person is able to build their hand eye coordination.
“More so than in a face-to-face physio exercise.
“It creates a scene that the person can engage with.
“That scene that we’ve chosen is because we know its of real interest to the individual.
“So for me for example it would be riding my bike. I may actually start to raise my hand a little bit reaching for the front handlebars.
Advertisement
Hide AdAdvertisement
Hide Ad“At the other end of the scale, for people who have an acquired brain injury or memory loss, it’s used for lose of people to relax, to be calm.
“Particularly with someone with memory loss there is that real anxiety or immediate fear of where am I who are these people.
“What the evidence base shows is that it reduces anxiety and tackles depression.”
‘Heather’s so precious to us. She’s brought a lot of love into the world’
Advertisement
Hide AdAdvertisement
Hide AdHeather is just like any other 27-year-old. As a teenager she had dreams of becoming a journalist, she loves her woo woo cocktails, nights out in Blackpool and enjoys an evening at a concert as much as the next person.
A bright student, she was among the top pupils at school and loved life, often taking part in rowing competitions as a sea cadet.
But when she was diagnosed with juvenile Huntington’s disease aged just 18, her life took a turn in a different direction.
Her grandfather George, 77, and grandmother Mildred, 78, looked after Heather and her twin brother Alex from the tender age of three months so that their mum could head out to work.
Advertisement
Hide AdAdvertisement
Hide AdAnd Heather still has a deep, loving relationship with her grandparents, who she sees at least once a month.
George, who lives in Fleetwood with Millie, said: “Heather’s very strong-willed. We have had some good laughs with her. She takes the mickey out of me. I used to sing to her and she would put her fingers in her ears.”
Looking back on Heather’s life, George went on: “Heather had a reasonably normal life until she was diagnosed in 2018. She was a very clever girl and loved her life. She joined the sea cadets at Fulwood and had a poem printed when she was about 14.
“She was very clumsy in her teens. That was the start. As soon as she started college she lost her concentration. It was Huntington’s coming on.
Advertisement
Hide AdAdvertisement
Hide Ad“She had to go to Manchester regularly for counselling for about 12 months before they diagnosed her. They won’t test them until they’re 18.
“She loves her cigarettes and chocolate. Heather is a lovely girl inside and out.
“Unfortunately she’s got this, it’s just so sad.
“She used to be able to come and visit us on a regular basis, but we visit her once a month now. They used to fetch her in between and we saw her every fortnight.
“She went into assisted living at Fleetwood and we just lived right around the corner.
Advertisement
Hide AdAdvertisement
Hide Ad“We were in and out all the time. We could take her out then. She could actually go out on her own.
“When she was in assisted living she wasn’t supposed to go out at night but she used to sneak out and get a bus and go to Blackpool.”
And George says its tough to know what lies ahead for his granddaughter.
“It’s a 10 to 15 years life span from diagnosis and it’s so diffcult for her.
Advertisement
Hide AdAdvertisement
Hide Ad“At school she started to do some part-time work. When she couldn’t carry on with college she worked in a store in Fleetwood.
“She gets Employment and Support Allowance now which helps her. She’s very brave girl.
And Heather still managers to see her favourite band.
“She loves One Direction. I’ve managed to get her to two of their concerts in Manchester. She also went to Lytham Proms to see George Ezra and she’s been on a couple of holidays to Blackpool.
“She gets wonderful care at Cuerden. She’s got good friends there as well. She’s accepted what’s going to happen to her. She knows her condition as far as her life span and everything. We’ve already taken steps to find out what Heather wants for her end of life.
Advertisement
Hide AdAdvertisement
Hide Ad“It’s a burden shared. Millie and I love her to bits. We have had a few tears on the road.”
And George reveals he tried to get Heather onto a Huntington’s clinical trial.
“I managed to have a conversation with the man leading the trial but he said unfortunately she’s not up to doing it now. But there’s lots of trials going on all over the world for Huntington’s and some of them are looking good.
“I have tried to find something that will help, you never know.
Advertisement
Hide AdAdvertisement
Hide Ad“She’s so precious. She’s brought a lot of love into the world.”
HOW TO DONATEReaders are welcome to donate any amount to the appeal. Anyone who donates £10 or above will have their names included in our Sponsor a Star article in the paper, just before Christmas.To donate, go to www.sueryder.org/makeadonationOr send a cheque to:Lancashire Post Appeal, Supporter Care, Sue Ryder, 183 Eversholt Street, London NW1 1BU
Fatal illness Huntington’s is passed down from parents
Huntington’s disease is a condition that stops parts of the brain working properly over time. It’s passed on (inherited) from a person’s parents.It gets gradually worse over time and is usually fatal after a period of up to 20 years.The symptoms usually start at 30 to 50 years of age, but can begin much earlier or later.Symptoms of Huntington’s disease can include:* Difficulty concentrating and memory lapses* Depression* Stumbling and clumsiness* Involuntary jerking or fidgety movements of the limbs and body* Mood swings and personality changes* Problems swallowing, speaking and breathing* Difficulty movingFull-time nursing care is needed in the later stages of the condition. It’s usually fatal about 15 to 20 years after symptoms start.Huntington’s disease is caused by a faulty gene that results in parts of the brain becoming gradually damaged over time.You’re usually only at risk of developing it if one of your parents has or had it. Both men and women can get it.
One resident said ‘you made life worth living'
Sinead Gallery began her career in sports physiotherapy but seeing the difference it can make to people’s lives, she took a detour and is now focusing on working with people with neurological conditions.
Advertisement
Hide AdAdvertisement
Hide AdShe said: “One resident was told he would never be able to walk again and he’s up and using a walking frame at the minute.
“It’s his family as well. Obviously being told at the hospital that you’re never going to be able to walk again and then for his family to see him walking is amazing. It just gives him that little bit of hope.
“Not everybody is going to be able to get up and walk again but just being able to reach for the phone or something like that, it’s amazing.
“I’ll never forget one resident we had.
“He said ‘the doctors made it so that we can live but you made it worth living’ and that’s stuck with me since.
“It made me cry when he told me. It’s a privilege as well gaining their trust. It just makes your job worth doing.”