More hospital patients ‘waking up during surgery’
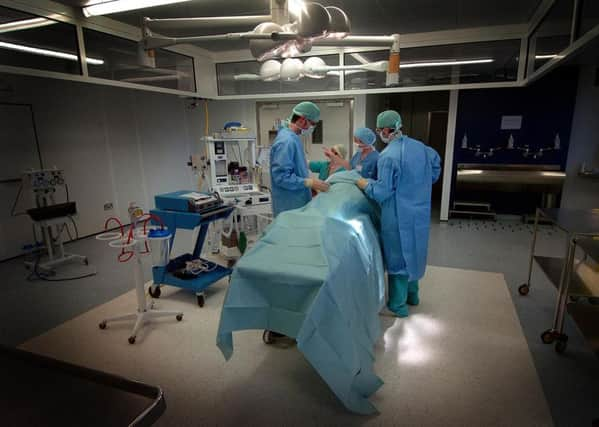

The phenomenon, known as Accidental Awareness during General Anaesthesia (AAGA), is one of the most feared complications for people who are put under general anaesthesia during surgery and patients may experience sensations of choking, suffocation and panic, and even fear they are going to die.
The use of muscle relaxants, which are required for safety during surgery, are likely to mean they are unable to communicate the fact that they are awake to the surgeon so they can only lie there helpless.
Advertisement
Hide AdAdvertisement
Hide AdA report by the Royal College Anaesthetists last year found around one patient in every 19,000 reports AAGA after being put under general anaesthetic, amounting to nearly 160 patients a year.
But researchers said that figure was based on patients pro-actively coming forward and reporting their experiences to hospital authorities, indicating that the real number was likely to be as much as 10 times as many.
They also said certain groups of people are more at risk of premature awakening, including pregnant women and patients who are morbidly obese, have certain infections, liver disease, malnutrition or are in the advanced stages of cancer due to the challenges their health issues pose to anaesthetists.
Scientists in Denmark carried out a study on patients with a condition called BChE deficiency - a rare metabolic disorder characterised by prolonged paralysis after the use of certain muscle relaxing drugs.
Advertisement
Hide AdAdvertisement
Hide AdThey interviewed 123 patients with BChE deficiency who had had a general anaesthetic for surgery and found that 89 of them (72%) suffered premature awakening, becoming conscious while still paralysed by neuromuscular blocking drugs.
They said that when neuromuscular monitoring was used - which measures how well a patient’s muscles are able to function during the surgery - 14 patients (29%) suffered the same condition but when it was not used, 100% of patients interviewed suffered accidental awareness and premature awakening.
Professor Jennifer Hunter, vice president of the Liverpool Society of Anaesthetists, said better monitoring of neuromuscular drugs would help to protect those patients who are at risk. Separate research has found that only around half of European anaesthetists use neuromuscular monitoring.
She said: “This study focused on a small group of patients with a rare genetic enzyme deficiency, but it is important to realise that other groups could be similarly affected, including pregnant women, patients with advanced cancer and those who are morbidly obese.
Advertisement
Hide AdAdvertisement
Hide Ad“While the vast majority of patients suffer no complications during anaesthesia, we simply don’t know how many people are affected by accidental awareness or premature awakening.”
Professor Hugh Hemmings, special edition editor of the British Journal of Anaesthesia, where the study is published, said: “T he real numbers of patients experiencing accidental awareness could easily be twice that figure.
“And given the numbers of unreported cases, it could be as high as tenfold that figure, especially among the highest risk patients.”