How Preston medics helped a patient barely able to breathe for three years - when nobody else could


He credits the treatment he received there for giving him his life back and has now returned to thank the staff responsible - and the doctor who listened to him.
Dr. Aashish Vyas leads the Airways team at the hospital and diagnosed a condition in Iain which had left specialists elsewhere stumped.
Advertisement
Hide AdAdvertisement
Hide AdThe reunion was the result of a presentation Iain gave to the board of the trust which runs the Royal Preston, in which he stressed the importance of medics hearing what their patients have to say.


“Dr. Vyas was the first doctor who had listened,” Iain says. “He knows the human body better than me, but I know my body better than him.”
And Iain was convinced that his difficulty breathing was not stemming from his lungs, but his throat.
At the age of 37, the fit and active father-of-two returned home from work one day in July 2015 and, within moments, his life had changed.
Advertisement
Hide AdAdvertisement
Hide Ad“I had something to eat and that was it - I suddenly couldn’t breathe and couldn’t move.”


But it would be over two and a half years before Iain found out what was wrong. During that time, he was seen by doctors at two different hospitals in the North West and was tested for everything from cancer to Aids.
The first nine months after he fell ill were spent in and out of hospital, including spells in intensive care. “The nurses knew my name,” Iain recalls.
But in spite of the severity of his symptoms, he was always eventually discharged with nothing more than nebulisers and steroids, because nobody could diagnose the problem.
Advertisement
Hide AdAdvertisement
Hide AdThe former warehouse worker had to give up his job and could no longer be the father he wanted to be for his two young children. “A trip to Stonehenge wiped me out for four days. My daughter used to cry when she saw me [suffering],” Iain remembers.

His life finally changed when he was referred to the Airways team in Preston six months ago, where a diagnosis was delivered within an hour - after nearly three years of delay.
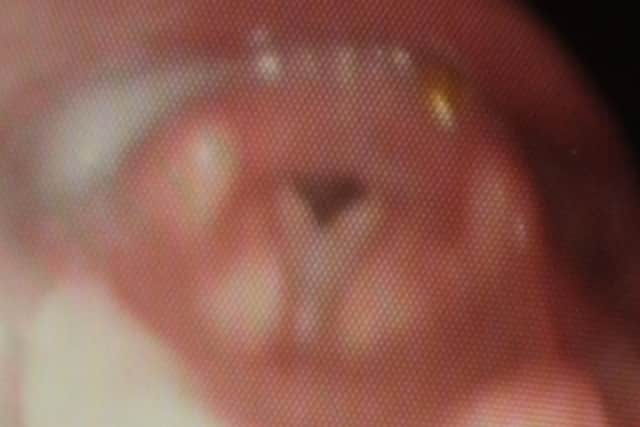
Dr. Vyas ordered a nasal endoscopy, which involves inserting a camera into the patient’s nose. The result came as no surprise to the consultant - it revealed a condition called Induced Laryngeal Obstruction (ILO).
Iain had been right - the root of the problem lay in his larynx at the back of his throat.
Advertisement
Hide AdAdvertisement
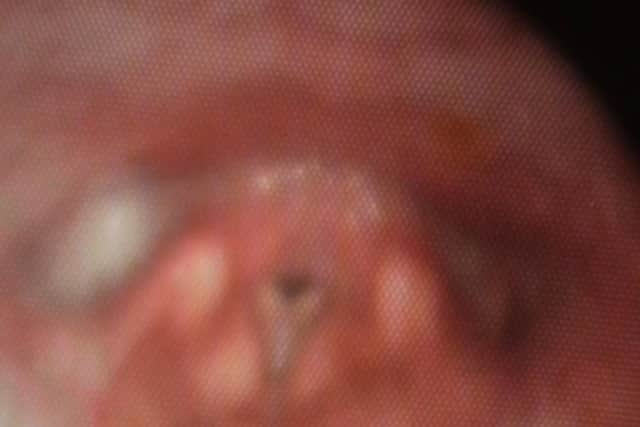
Hide Ad“In patients with ILO, the voicebox shuts down, so air literally cannot go in through your nose and into your lungs,” Dr. Vyas explains.

“We see up to 450 patients a year with very severe problems breathing. Sometimes it is misdiagnosed as asthma - or sometimes they do have asthma, but also other complicating factors which make [their] breathing problems resistant to normal therapy.”
It is thought around 10 percent of the 5.4m people diagnosed with asthma in the UK instead have ILO, meaning inhalers will not have any effect.
But a third of asthma sufferers have ILO as well - and the nature of the condition means the medication needed to treat their asthma cannot get to where it is needed.
Advertisement
Hide AdAdvertisement
Hide AdIn Iain’s case, he emptied 55 inhalers in just over two years - but now barely needs to use them.
“We try to reduce the burden of medication,” Dr. Vyas explains. “For the health economy - but, more importantly, for the patient - the outcome is much better.”
And the involvement of the Airways specialists does not end with diagnosis. That is the point at which what Dr. Vyas describes as the “compassionate soul of the service” steps in.
Claire Slinger is the department’s consultant speech and language therapist - one of only two at that grade in the country. She and her team train patients in the breathing techniques they need to adopt in order to live with ILO.
Advertisement
Hide AdAdvertisement
Hide Ad“There are certain triggers [for an attack], such as physical strain or the smell of perfume,” Claire explains.
“The exercises retrain the voicebox to be more open. We don’t want to create dependence on us, we want to be able say, ‘You have this condition - this is what you need to do to manage it’.”
The Royal Preston is one of just three hospitals in the country specialising in the diagnosis and treatment of ILO.
And that makes Iain one of the lucky ones - patients elsewhere in the country wait an average of nine years before the problem is even identified.
But for Dr. Vyas, the key is to go back to basics.
Advertisement
Hide AdAdvertisement
Hide Ad“The best thing is to listen to your patient,” he says. “Strip everything back and try to find out what’s gone wrong.”
It is an approach which came as a breath of fresh air for Iain - and gave him a new lease of life as he turned 40.
“I was trapped in my own body, unable to breathe,” he says. And a simple breathing technique has transformed me.
“I can’t stop smiling. Anything that happens now in my life is down to Dr. Vyas and his team.”
What is ILO?
Advertisement
Hide AdAdvertisement
Hide AdInduced Laryngeal Obstruction (ILO) was first identified in 1994 and often results in sufferers feeling as though they cannot breathe. It can stem from a viral infection and is brought on by exercise or certain other triggers like scents.
Jessica Blakemore, a speech and language therapist at the Royal Preston Hospital, explains:
“ILO patients are experiencing closure of the vocal cords when breathing. So when the patient breathes in, instead of the vocal cords opening up - to allow airflow through to the lungs - they are staying quite tight and that’s making breathing more difficult.”
Other symptoms include voice problems, chronic cough or the feeling of choking.
Advertisement
Hide AdAdvertisement
Hide Ad“The first thing I am trying to understand is what makes their breathing different to asthma,” Jessica explains. “A lot of people who come through our doors have a misdiagnosis [of] asthma, or they have asthma as well.
But as the Royal Preston’s consultant speech and language therapist Claire Slinger warns, “The worst thing that can happen with ILO is that a patient passes out, but asthma can be much more serious.”
Yet ILO sufferers can often feel as though they on the verge of something far worse than fainting.
“When people are experiencing an acute attack - especially if they don’t understand what’s happening - they can think, ‘I’m going to die’,” Jessica says. “Reassurance is a massive part of what we do.”
Advertisement
Hide AdAdvertisement
Hide AdChildren who are affected by the condition often give up exercise, because they are scared of the symptoms.
Diagnosis can be made only by inserting a camera up the patient’s nose - at the time they are experiencing symptoms. That means Jessica has to try to induce the problem - usually with a spray of deodorant or the scent of nail varnish remover.
Once ILO is confirmed, patients are given breathing exercises to retrain the key muscle which causes the larynx to open.