Go-ahead for new staff to ease pressure at the Royal Preston and Chorley hospitals
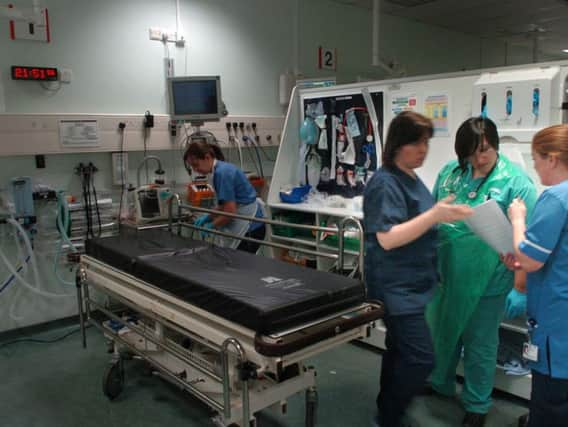

Extra nurses will be brought into the Accident and Emergency unit at the Royal Preston and the children and young people’s departments across both sites.
Preston’s A&E will get almost 15 additional full-time equivalent posts, some of which will be deployed in the three new areas which have recently opened in the unit - including a rapid assessment facility for triaging patients when they first arrive.
Advertisement
Hide AdAdvertisement
Hide AdThe extra 20 full-time equivalent staff in the children’s departments will include a paediatric nurse to be stationed during peak periods at both of the region’s A&E units.

The additional cash comes in spite of a previous investment of £8.4m during 2017/18 not bringing staffing up to the intended level.
But board members were told that the money had been spent covering shifts with temporary staff to ensure patient safety.
“There have been many positive outcomes of that investment - including improved ratings [from the regulator] and better patient experiences,” Gail Naylor, nursing and midwifery director, told a meeting of the trust’s board.
Advertisement
Hide AdAdvertisement
Hide Ad“We have been able to demonstrate that where we have managed to recruit [the necessary] staff, those staff have a much more positive experience - and that leads to them staying with the trust.”
Members heard that the trust was not expecting to have difficulties recruiting the latest crop of additional staff - because of the popularity of the posts which would be on offer.
Staffing levels are dictated, in part, by national guidelines. But every ward and department has been asked for its input on the numbers required in their own areas.
Tim Watkinson, a non-executive director of the board, asked for reassurance that “the natural desire to increase rather than to scale back” had been challenged.
Advertisement
Hide AdAdvertisement
Hide AdSarah Cullen, deputy director of nursing, said the process had been “rigorous” - and had involved the deployment of new roles to overcome a national shortage of registered nurses.
“More often than not, staff will say they need more. And while it is not always appropriate to take out [staff numbers] in their entirety, there are opportunities for safe approaches to efficiency,” she said.
The introduction of alternative roles like nurse associates and discharge facilitators - to speed up the process of getting patients out of hospital - has contributed to £532,000 in savings on staff. Twelve full-time equivalent roles have been removed from the wards.
That has reduced the overall level of additional investment required in nursing staff across the trust from £1.3m gross cost of the new positions to the £854,000 which now needs to be found.The trust’s annual nursing staff bill will stand at £61.8m after the new staff have been recruited.
Advertisement
Hide AdAdvertisement
Hide AdThere will also be an increase in the number of beds in the critical care unit from 14 to 16.
Papers presented to the board reveal that the additional capacity will reduce the risk of complex procedures having to be cancelled.
It will also generate an extra £223,000 each year for the trust by allowing more operations to go ahead for patients who may need intensive care afterwards.
Staff to patient ratios at the trust range form 1:1 in critical care through to 1:4 in acute assessment areas and 1:8 on general wards.
The ratio can increase to 1:13 on general wards overnight.