A&E staff at Royal Preston Hospital left 'crying with frustration' as patients 'die without dignity' in crowded waiting rooms
and live on Freeview channel 276
A&E clinical director Graham Ellis, matron Tracey Thorn, and managers Clare Holbourn, Doberah Lealman and Rachel Standeven wrote to executive team at Lancashire Teaching Hospitals Trust about their concerns about the safety of the hospital’s emergency department on March 30, as ‘the current situation is worse than it has ever been’.
They said: “For the past few months we have on a regular basis had more than 50 patients waiting for a bed and that wait being in excess of 60 hours. This means at times there is little or no space to accommodate new acutely ill patients, causing ambulance handover delays of over four hours and delay in treatment. Patients, often elderly with multiple co-morbidities, have to sit in the waiting room, some for over 24 hours waiting for a cubicle space and treatment. Patients wait outside the department as there is no space to socially distance in the waiting room.
Advertisement
Hide AdAdvertisement
Hide Ad"We all know from GIRFT (a national programme designed to improve the treatment of patients) data that patients die as a direct result of long waits in ED. Morbidity also increases and we are seeing this in patients with an increase in clinical incidents, pressure sores, delayed treatment, detrimental outcomes, datix and complaints. This has a huge impact on members of staff who are working extremely hard but complete their shifts knowing they haven’t provided the care that they would want to, physically and mentally drained, and despite their best efforts have seen patients suffer and have received negative comments from distraught relatives and carers.
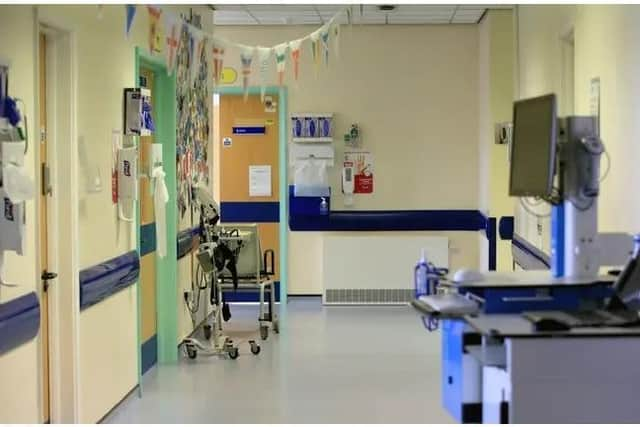

"We have witnessed senior staff crying with frustration and anger as they have had to resuscitate patients in the waiting room, examine in the viewing room and CT changing room, seen patients leave the department as they have been pulled out of a cubicle to allow someone more unwell to be treated in their former space, and patients die without the dignity of privacy. All this on the back of a two year pandemic, screening patients, constantly shifting treatment spaces due to Covid status and relaying messages to family members who cannot be with their loved ones. The medical and nursing coordinators often leave their shifts late, feeling guilty with what they have handed over and upset with the compromises they have had to make."
They added: “The culture of the Trust has not changed – ED is still the fall back for everyone. Each ward and assessment area can claim full or have criteria preventing admission. ED apparently has a never ending elasticity in the eyes of others… all roads lead to ED.
"There are criteria for surge when we are near capacity. It rarely works – we remain full. There is not the staff and there is not the response at the required urgency. We often hear there are no beds and no movement and no further options. This is not good enough.”
Advertisement
Hide AdAdvertisement
Hide AdThe Lancashire Teaching Hospitals NHS Foundation Trust was approached for comment.
However, Kevin McGee, the trust’s chief executive, said in a statement to the Health Service Journal: “The safety of patients and the welfare of staff remain the trust’s top priorities and we would like to express our ongoing thanks to our emergency department colleagues who continue to demonstrate commendable resilience and compassion to each other and our patients in very challenging circumstances.
“Like NHS providers across the country, our hospitals have continued to sustain unprecedented pressure which has been exacerbated by the covid-19 pandemic.
“Lancashire Teaching Hospitals has established and robust processes in place to ensure patient safety and discussions have taken place between emergency department clinicians and trust leadership to help collectively agree approaches to reduce the impact of concerns raised.”