Why do only 50% of GP surgeries offer extended access?
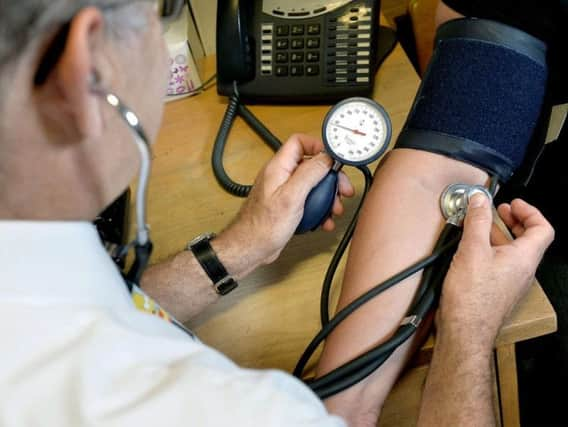

And figures reveal there are more than 170,000 people across Lancashire without any access to their own doctor’s practice in the evenings and at weekends, while a further 750,000 are only getting part of the service pledged four years ago.
Patients were promised they would soon be able to book doctors’ appointments in the evening, at weekends and before the working day started in order to fit in with increasingly busy lives.

Advertisement
Hide AdAdvertisement
Hide AdBut now our investigation reveals in Preston just 50 per cent of surgeries offer full extended access, with 59.4 per cent of patients having the opportunity to book out-of-hours appointments right through the week.
And in Chorley and South Ribble the picture is even worse – with only 34 per cent of practices offering extended opening compared to 55 per cent in Fylde and Wyre.
However, in some areas schemes are in place to allow patients to see an out of hours GP at another practice – although in some cases the nearest one may be several miles away.
The extended access was not intended for emergencies, but for people to be able to make routine appointments with their GP without taking time off work.
Advertisement
Hide AdAdvertisement
Hide AdThe figures also show the post code lottery for people living in Lancashire, with huge variation in the level of service offered both within the county and nationally.
Rollout of the full extended access service ranges from 90 per cent in Blackburn with Darwen to just 10 per cent in West Lancashire.
Meanwhile three clinical commissioning group (CCG) areas – Fylde and Wyre, Blackburn with Darwen and West Lancashire – have at least a partial out of hours service for patients at all surgeries. Yet in East Lancashire more than 22 per cent of patients have no extended access at all.
And most of the county remains far behind other parts of England – and the NHS’s target of total rollout by October this year. NHS England says it is on track to hit this target.
Advertisement
Hide AdAdvertisement
Hide AdPatients in Lancashire generally fare slightly better than the national average, which showed that 40 per cent of practices offered full extended opening, but worse than many boroughs in London and the South East, where almost all surgeries offered the provision. In total there are 24 out of 207 areas – including Blackburn – where more than 90 per cent of patients have full access to extended opening.
David Blacklock, CEO of Healthwatch Lancashire, said: “Many of us have commitments in our everyday lives which impact our ability to access health care within normal working hours – work, childcare etc – meaning the need for services to be more patient-centred has never been greater.
“The Government made a commitment to enable people to access care when they need it. This clearly is not reflected in people’s experiences.
He added that CCGs locally are “still some way short of the Government target of 90 to 100 per cent provision”.
Advertisement
Hide AdAdvertisement
Hide Ad“NHS leaders must ensure that the views of patients are taken into account as they shape and improve services and clearly must do more to make these services responsive to patient needs,” he said.
An NHS England spokesperson said: “The NHS is investing at least £258m this year to offer improved access to general practice, including evening and weekend appointments.”
They added that the publicly available figures used in this investigation – collected by the BBC’s Shared Data Unit and analysed by The Post – “collects information on extended access from individual GP practices” and does not include those who provide the service as part of a “hub” of surgeries – as happens in parts of the county.
The data is collated bi-annually from surveys filled out by individual GP practices. It found 41 per cent of GP practices in England offer full provision for extended access, with 40 per cent of patients were registered at a practice offering full provision to extended access.
Advertisement
Hide AdAdvertisement
Hide AdNHS England said its own analysis shows out of hours access now stands at 55 per cent nationally but did not provide the data this was based on.
The national picture
With extended access, appointments are defined as scheduled slots with a GP, nurse or member of general practice staff providing direct patient care. Appointments must be pre-bookable.
In England, ‘extended access’ is delivered by CCGs through individual GPs practices or through hubs or federations.
Full provision means patients have access to pre-bookable appointments on a Saturday and Sundays and on each weekday for at least 1.5 hours in the early morning from 8am and in the evening after 6.30pm through the practice or a group of which the practice is a member.
Advertisement
Hide AdAdvertisement
Hide AdPartial provision means patients have access to pre-bookable appointments on at least one day a week, through the practice or the practice group, but the extended access offered is not sufficient to meet the criteria of full provision. The minimum provision to meet this criteria is 1.5 hours once a week.
A Department of Health spokesman said: “We want everyone to have access to GP services, including routine appointments at evenings and weekends - and already millions of patients have benefitted from this which is backed by our investment of an extra £2.4 billion a year into general practice by 2021.”
The Shadow Secretary of State for Health and Social Care, Jonathan Ashworth MP said: “This is yet more evidence that the Tories have broken their promises on access to GPs seven days a week.
“The truth is that years of austerity has taken its toll on general practice. We need a serious long term investment plan for primary care.”
Advertisement
Hide AdAdvertisement
Hide AdThe British Medical Association’s GP committee chairman, Dr Richard Vautrey said: “While schemes like this (extended access) are rolled out and are successful in providing the services they are commissioned to do, we still believe the money invested in such programmes would be better spent improving core GP services.
“We know that patients are frustrated with being unable to get timely appointments during regular working hours, owing to increased demand and unmanageable GP workloads, and therefore it is these services that should be a priority for proper funding.”
