Seriously ill grandmother forced to have swabs and blood samples taken next to toilet at Chorley Hospital
and live on Freeview channel 276
Enid Roberts, 84, of Lostock Hall, was left for more than three hours in what her family describe as “absolute chaos” in the Medical Assessment Unit (MAU) at Chorley Hospital on Wednesday evening.
Even though medics said she needed to be in isolation because of her illness, Mrs Roberts was kept in a busy thoroughfare due to a lack of available rooms and was only given a mask an hour after arriving.
Advertisement
Hide AdAdvertisement
Hide AdFor two-and-a-half hours she was kept lying on the ambulance stretcher she arrived on, on the advice of medics - meaning paramadics were unable to get to other jobs - and only moved onto a chair when the paramedics had to go back to Preston when their shifts finished.
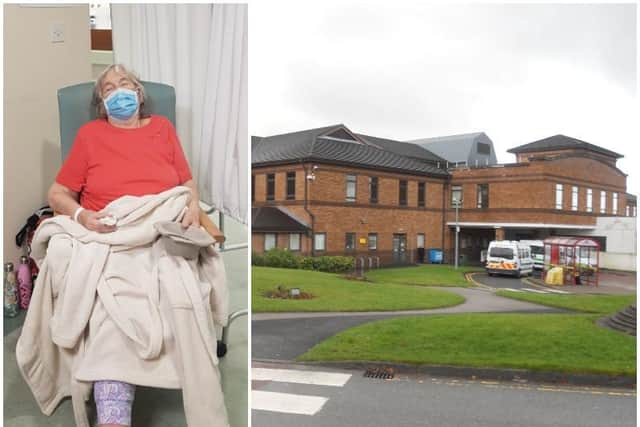

Daughter Alison Holgate, 53, said: “It was a very distressing situation, absolute chaos.
“The doctor who carried out a home visit earlier in the day was told by the hospital that she’d be taken straight up to her own bed in the MAU - I heard the phone call. But it didn’t happen. It was like walking into a war zone.”
She said: “It would be wrong to describe it as a corridor. It was an annexe, a square about 7ft by 7ft, with toilets either side, a relatives room, a brew room for staff and a dirty utility room.
Advertisement
Hide AdAdvertisement
Hide Ad“She had bloods taken in a chair there and a consultant was asking very personal questions about things like bowel movements, when people were walking passed with bed pans, members of public were knocking about and could hear everything. There was absolutely no dignity there.


“It was very unpleasant and probably unhygenic. I’m glad that my mum was out of the game really, because she would have been upset by it all.”
Mrs Roberts, who used to run a paper shop in Pall Mall, Chorley, was eventually moved into an isolation room at around 7.15pm, where her family have been told her condition remains “very low”.
Mrs Holgate, who works with offenders, said: “It’s not the staff that we’re upset with, it’s the mismanagement of it all. When we got there, one of the sisters said to me ‘I could cry, I’ve nowhere to put her’.
Advertisement
Hide AdAdvertisement
Hide Ad“I complained to the Trust and was given a phone number for the PALS (Patient Advice and Liaison Service), but that closes at 4pm, so what good is that?
“I did say that I might have come across as a bit irritable, but I defy anyone to see their mum in that state and not do anything about it.
“If people don’t complain about these things, then nothing will ever change.”
Mrs Holgate has also contacted hospital governor Pav Akhtar about the situation, who replied to her via social media, stating: “I’m sad to see this. That picture speaks a thousand words.
Advertisement
Hide AdAdvertisement
Hide AdNo patient should be subject to this experience in the NHS. No family should need to photograph a loved one to show it happened. I apologise for the distress and will escalate via @LancsHospitals. I hope mum’s stable now.”
Karen Partington, chief executive of Lancashire Teaching Hospitals NHS Foundation Trust said: “All suspected and confirmed patients with influenza do get isolated as soon as possible. We are working together with all wards in regards to flu management, and correct procedures for suspected flu and confirmed flu positive patients.
“We encourage anyone that has concerns whilst in our care to contact the Patient and Liaison Service (PALS) team so they can support patients, relatives, and carers to resolve any issues with care promptly.”
Tens of thousands wait more than four hours
In October the Post revealed that tens of thousands of A&E patients at Lancashire Teaching Hospitals waited more than four hours to be seen last year.
Advertisement
Hide AdAdvertisement
Hide AdThe figures for the Royal Preston Hospital and Chorley Hospital were in line with the national picture, with medical experts blaming a combination of staff shortage, lack of funding, and increased demand for rising waiting times across England.
NHS data shows that A&E patients at Lancashire Teaching Hospitals NHS Trust - Royal Preston Hospital and Chorley Hospital - were left waiting more than four hours on 27,212 occasions in 2018-19.
It means that 83 per cent of around 157,000 attendances were admitted, transferred or discharged within four hours of arrival – well below the NHS’s target of 95 per cent.
The proportion of patients seen within the target time at the trust has dropped significantly in recent years – the figure stood at 95 per cent in 2013-14.
Advertisement
Hide AdAdvertisement
Hide AdNHS bosses recently unveiled plans to scrap the four-hour standard – introduced in 2004 – after arguing it was outdated due to the changing nature of emergency care.
It proposed replacing it with four new targets, including a focus on the most critically ill and injured, and measuring the average waiting time for all patients.