Preston's 'robo-surgeon' hits the 500 mark in two years
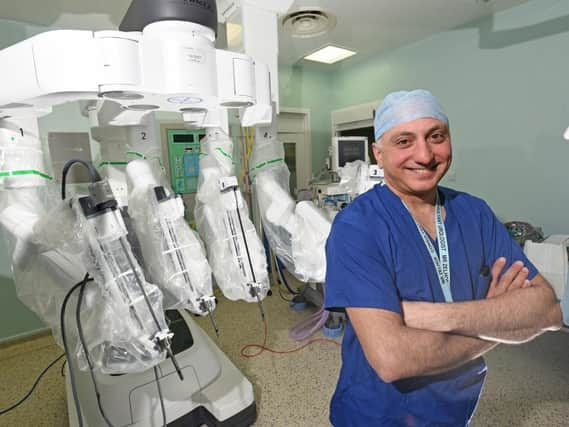

The DaVinci Xi is the most advanced robotic surgical system on the market and was bought by Rosemere Cancer Foundation with money donated by the public.
The robot is used at the Rosemere Cancer Centre at Royal Preston Hospital to operate on patients with bowel, gynaecological and urological cancers.
Advertisement
Hide AdAdvertisement
Hide AdIt was first used on a patient on May 3, 2017 and to date, more than 530 patients have been treated with the Xi.

When it arrived, it was the first of its kind in the whole of the North of England and one of just three in the entire country, the others being at the Royal Marsden Hospital in London and a hospital in Birmingham
The city now has one of the UK’s biggest robotic surgery case lists – a shift credited with improving not only patient outcomes but also saving Lancashire Teaching Hospitals NHS Foundation Trust thousands of pounds that it can spend on other aspects of patient care.
The Xi provides a three dimensional view of the area to be operated on via a computer console that is linked to arms that end in jointed “wrists” that can turn 360 degrees and are with fitted tiny instruments that can cut with such precision they can peel a grape without damaging the flesh beneath.
Advertisement
Hide AdAdvertisement
Hide AdSurgeons can therefore access parts of the body that are difficult to reach and undertake complex procedures using keyhole incisions rather than having to “open up” patients, causing a wound.
The main patient benefits of keyhole surgery over open wound surgery are a faster recovery time, less post-operative pain and a reduced risk of post-operative complications.
Patients having operations that with standard open wound surgery could expect to be in hospital for two to five days are generally home within 24 to 48 hours of admittance if operated on with the Xi.
This is not only beneficial to patients and their families but also to the Trust, as the cost of a bed is £350 per day.
Advertisement
Hide AdAdvertisement
Hide AdBachar Zelhof, consultant urologist surgeon, uses the machine to perform surgery on the kidney.
He said: “When we first started, patients were initially apprehensive because they thought the robot was in charge and I would be elsewhere having a coffee, but that is not the case. The surgeon operates, but we are using robotic instruments because it offers better movement and vision.
“It is much more accurate and safer. No matter how steady your hands are, they can shake. The robot gets rid of that.”
Mr Zelhof likens operating the machine to ‘playing the organ.’
Advertisement
Hide AdAdvertisement
Hide AdHe added: “You need the same type of co-ordination as when you plan the piano or organ. You use your feet to operate the camera and your fingers to control the movement of the instruments.
“The robotic arms have various instruments attached, such as scissors, forceps or staples and these go into the patient’s abdomen to make an incision.
“The surgeon goes to the console and the scrub nurses and assistants are next to the patient, changing the instruments as instructed.
“The surgeon has a 3D view of what is happening, so they can see the margins around the cancer and accurately pin point. With previous key hole surgery (laparoscopy), it was 2D, which was not as clear.
Advertisement
Hide AdAdvertisement
Hide Ad“For kidney surgery, the procedure is about three to three-and-a-half hours.
“Because of the accuracy, the surgeon can remove the tumour and leave the rest of the kidney in tact, which maximises its function and is better for the patient.”
As a result of the precision and ease of the procedure, the team at Rosemere are using the robot more and more.
Mr Zelhof said: “We are doing more and more difficult cases which we would not have done with the previous keyhole surgery.
Advertisement
Hide AdAdvertisement
Hide Ad“We will need another robot at some point to keep up with demand. Once you have started doing it and see the benefits for patients, you don’t want to go back.
“We rarely do keyhole surgery now.”
Ioannis Peristerakis, is a consultant in Upper GI and Colorectal, performing surgery on the oesophagus, stomach and small intestine, as well as the bowel, colon and rectum.
He said: “The robot has different technologies that allow us to operate in a safer way and helps patients recover quicker.
“We have better vision, so we can operate on rectal cancers deep in the pelvis in a way that allows us to protect certain nerves in the body which perform sexual and blood functions.
Advertisement
Hide AdAdvertisement
Hide Ad“It also allows us perform the same quality of operation for patients who are obese and overweight.
“It is difficult for a patient to compare previous keyhole procedures as they will only have this operation once in their lives, but they appreciate the difference and benefits.
“The procedure makes patients feel like they are having a medium operation, rather than major and they feel much better afterwards.”
‘Op prevented kidney loss’
Sarah Rigby, of Penwortham, says she would have had to have one of her kidneys removed if she had not had the robotic procedure to remove a benign tumour.
Advertisement
Hide AdAdvertisement
Hide AdThe 49-year-old mother-of-two says: “I had a pain in my side, but I blamed it on other things, such as bad posture, so I kept putting it off.
“But it got worse towards the end of last year and I began feeling unwell and was not sleeping very well.
“It affected my appetite and I had an ultra sound on my abdomen in November. Doctors found something in my kidney so I had a CT scan, which revealed an abnormal tumour.
“As a result, I was referred to Mr Zelhof and had the operation in January.
Advertisement
Hide AdAdvertisement
Hide Ad“I was under general anaesthetic for three hours and I spent two days at Royal Preston Hospital.
“At first, doctors thought they would need to take away part of my kidney, but because the tumour was in the centre and the surgeon used the robotic procedure, he was able to remove the tumour instead.
“As a result, I was left with a fully functioning kidney with the tumour taken away.
“If it had not been for the robot, I would have had to have open surgery and the whole kidney removed.
Advertisement
Hide AdAdvertisement
Hide Ad“I feel really lucky that I live in the area where the robot is available. I can never thank Mr Zelhof and the team enough for everything they have done for me.
“It was fortunate that the tumour came back benign and was not cancerous.
“The staff on the ward at Royal Preston Hospital were so kind and lovely.”
Bowel cancer treatment
Nicholas Kos, of Clayton-le-Woods, was taken aback when the words ‘robotic surgery’ were uttered.
Advertisement
Hide AdAdvertisement
Hide AdBut when he was told all about how it works, he felt more assured.
The 59-year-old father-of-three says: “I had noticed some subtle changes in my bowel habits and after I spoke to my GP, a test conformed I have bowel cancer. I was referred for an endoscopic, which established I had a tumour. I was told there and then. That was exactly a year ago.
“Everything moved pretty quickly, I had four cycles of chemo which shrunk the tumour and I was scheduled for the robotic surgery in September.
“That was the first I had heard of that. It’s a pretty devastating thing to be told but once the first two week period has passed and you get feedback on what is happening, everything seems to improve a bit. I had to get on and I decided I would fully accept what they recommended without any questions.
Advertisement
Hide AdAdvertisement
Hide Ad“Using the robotic equipment, the surgeon, Ioannis Peristerakis, knew exactly where the tumour was and what he was going to do.
“I had a piece of my colon removed and then the two free ends were stitched together. The surgeon took the lymph nodes out that may have been affected.
“I felt groggy for a few hours after my surgery, but the next day I was feeling better. I was just a bit sore. And the day after that I was home.
“I had follow up appointments and doctors are happy the cancer had not spread so I have been discharged.
Advertisement
Hide AdAdvertisement
Hide Ad“Although it was a very frightening experience, it was a remarkable turn of events.
“I cannot speak highly enough of the people involved. They were fantastic.
“My advice to anyone who notices an changes in bowel movement or blood, to see their GP. The earlier it can be diagnosed and referred, the better.”
Preston’s robotic surgery
++ The robotic surgery was a number one priority in the trio of projects that made up Rosemere Cancer Foundation’s 20 Years Anniversary Appeal, which launched in March 2017.
Advertisement
Hide AdAdvertisement
Hide AdAn initial down payment towards its £1.25 million cost secured its arrival within weeks of the appeal’s launch
++ The surgical team using the Xi is made up of:
Tarek Hany, Consultant in Upper GI and Colorectal
Pierre Martin-Hirsch, Consultant in Obstetrics and Gynaecology
Ioannis Peristerakis, Consultant in Upper GI and Colorectal
Arnab Bhowmick, Consultant in Upper GI and Colorectal
Paul Turner, Consultant in Upper GI and Colorectal
Kish Pursnani, Consultant in Upper GI and Colorectal
Nick Wood, Consultant in Obstetrics and Gynaecology
Bachar Zelhof, Consultant in Urology
Pradip Javle Consultant in Urology
Blessing Dhliwayo Consultant in Urology
Michal Smolski Consultant in Urology
++ To date, they have undertaken the following operations:
Prostate 210
Kidney 100
Cystectomy 11
Colorectal 74
Gynae 110
Upper GI 29
They have been able to treat patients with a higher BMI (body mass index – obese patients) previously deemed unsuitable for keyhole/minimally invasive surgery
Other firsts and notables include:
++The region’s first day case hysterectomy
++The region’s first upper GI (gastrointestinal tract) robotic surgery
Advertisement
Hide AdAdvertisement
Hide Ad++ A combined robotic procedure to treat both bowel and womb cancer in the same patient
++ The recruitment of the first robotic patient into an international trial into rectal cancer
++ The Xi is made by an American company called Intuitive Surgery and it has designated the centre as one of its European centres of excellence and teaching hub for surgeons from across the Continent